Resources
- Breathing and Diastasis Recti: Understanding the Connection and Finding Relief
- Can You Have a Flat Stomach with Diastasis Recti?
- Ab Exercises for Diastasis Recti That Heal, Not Harm
- How to Choose the Best Diastasis Recti Program?
- Working Out with Diastasis Recti
- How to Fix Diastasis Recti Years Later: A Comprehensive Guide for Long-Term Healing
- Can Diastasis Recti Be Fixed Without Surgery?
- Is Diastasis Recti Preventable? | 5 Ways To Prevent Rectus Diastasis
- Diastasis Recti During Pregnancy
- Before and After: Diastasis Recti
- Can You Fix Diastasis Recti? Exercise Or Surgery
- What Does Diastasis Recti Look Like?
- Self Testing Diastasis Recti | 4 Simple Ways to Test Yourself
- Diastasis Recti Exercises | 8 Exercises for Rectus Diastasis
- Diastasis Recti Exercises For Men
- Diastasis Recti Surgery | Procedure Overview | Will You Need It?
- Is Diastasis Recti Fixable? | Exercise or Surgery
- Diastasis Recti Symptoms | Stomach, Back Pain, Pelvic Floor Issues

in this FREE video and get the support you deserve
*No spam, just quality
content and support
Resources
- Breathing and Diastasis Recti: Understanding the Connection and Finding Relief
- Can You Have a Flat Stomach with Diastasis Recti?
- Ab Exercises for Diastasis Recti That Heal, Not Harm
- How to Choose the Best Diastasis Recti Program?
- Working Out with Diastasis Recti
- How to Fix Diastasis Recti Years Later: A Comprehensive Guide for Long-Term Healing
- Can Diastasis Recti Be Fixed Without Surgery?
- Is Diastasis Recti Preventable? | 5 Ways To Prevent Rectus Diastasis
- Diastasis Recti During Pregnancy
- Before and After: Diastasis Recti
- Can You Fix Diastasis Recti? Exercise Or Surgery
- What Does Diastasis Recti Look Like?
- Self Testing Diastasis Recti | 4 Simple Ways to Test Yourself
- Diastasis Recti Exercises | 8 Exercises for Rectus Diastasis
- Diastasis Recti Exercises For Men
- Diastasis Recti Surgery | Procedure Overview | Will You Need It?
- Is Diastasis Recti Fixable? | Exercise or Surgery
- Diastasis Recti Symptoms | Stomach, Back Pain, Pelvic Floor Issues
Can Diastasis Recti Be Fixed Without Surgery?
By Lauren Ohayon 06/04/2024
6 Min Read
Healthcare professionals–including doctors, coaches, and doulas–have you been confused about how to help your patients and clients with diastasis recti? Is surgery the best and only option? Not necessarily. Read on to learn about strategies for the non-surgical repair of diastasis recti.
Table of Contents
Diastasis Recti and its Impact on Patient Well-being
Diastasis recti (DR) is the separation of the rectus abdominis muscles along the linea alba. While the majority of diastasis recti occurs during pregnancy, it can be found in other populations, such as athletes and people who were assigned male at birth. Most pregnant people experience some degree of DR at the end of their pregnancy; after a year, about 33% of postpartum people continue to have some degree of diastasis.
The symptoms of DR that your patients experience may include:
- Abdominal bloating
- Urinary or fecal incontinence
- Constipation
- Back pain
- Pelvic or hip pain
- Sacroiliac joint pain
- Lack of core strength and function
- Pain when walking or performing everyday tasks
A separation (under 22–30 mm) is usually not a functional issue. Although there is not a standard diagnostic distance, more than 30mm separation frequently impairs the core’s ability to engage effectively. The primary measure of core function for a DR is the ability of the linea alba to maintain tension under load. It’s possible to have a relatively wide but shallow diastasis that is better able to function than a narrow, deep separation.
Wider separations often also make a psychological impact on patients, as the internal organs may bulge into the space between the abs and create a visible dome or ridge along the midline. While this is usually an aesthetic concern, your patients may need therapeutic support in managing their feelings about their body as they heal the injury.
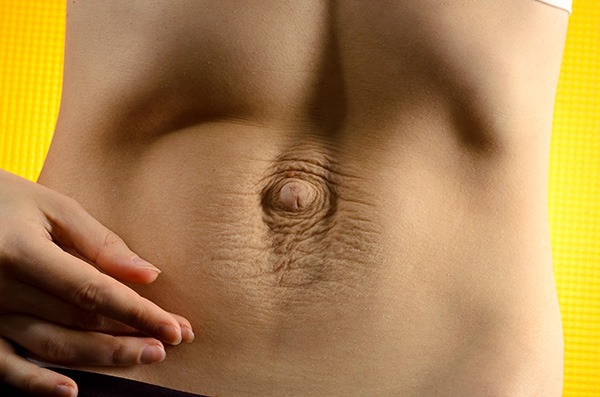
Can diastasis recti be fixed without surgery?
The choice for surgical repair depends on the person’s perception of their symptoms, and if they are interfering with quality of life at an unacceptable level. Most medical plans (whether private insurers or governmental healthcare entities) consider surgery to be a cosmetic procedure in most cases of DR. Surgery may be covered if specific criteria are met, including width, impact on activities of daily living, and evidence that the patient has done a trial of physical therapy for 6 months to a year with no discernable results. The specifics vary from country to country, so you may wish to do research depending on your locality.
The first line of treatment for diastasis recti is physical therapy for at least 6 months for good reason–the symptoms of diastasis recti are generally responsive to targeted exercises that strengthen the core.
“[…] during the early post-natal period, exercises might be highly effective, making this a possible nonsurgical solution for DRA. Static abdominal contractions, pelvic rocking, sit-up and leg slide exercises are also recommended for a stubborn and protruding abdominal wall. Bilateral activation of the transversus abdominis can reportedly stabilize the ribs, linea alba and thoracolumbar fascia. Engaging the transversus abdominis shortens the rectus abdominis muscles and brings together the gap at the linea alba
However, not all bodies respond equally well to exercise, and if a regular core-training regimen has been undertaken without success, there are several surgical routes that involve reducing the width of the stretched tissue of the linea alba” (Thabet, 2019).
Numerous studies have shown that there are few differences in terms of long-term outcomes among different types of surgical repair. One study indicates that incorporating core training both before and after surgery can significantly increase the overall effectiveness and long-term success of surgical outcome: “The study showed significant improvements in function. The self-reported symptoms of back pain, abdominal pain, core control, core weakness, bulging, constipation, urinary incontinence, and cosmetic issues showed significant improvements at the 1-year follow-up. The two most common symptoms reported before surgery were back pain and lack of core control, and these also showed the greatest improvement at follow-up. Even though symptoms before and after surgery were registered as dichotomous yes/no answers, the findings reflect the panorama of functional disabilities reported in previous studies (Olsson et al., 2023).
In general, patient satisfaction is high with surgery, although, as Olsson et al. (2023) suggest, “The self-reported symptoms, bulging, and cosmetic issues significantly improved but remained to some extent. These ‘body image’ symptoms may need specially designed management. In cases with severe abdominal wall insufficiency, [rectus diastasis] repair alone may not be sufficient.” In other words, even if the DR is repaired, we need to keep in mind that body image issues can make a sense of “healing” difficult to access for some people.
While some cases of DR may require surgical intervention, the vast majority respond well to exercise. Non-surgical methods not only empower patients by making them feel strong and more capable physically but also have a well-documented positive impact on mental health. Additionally, with adequate counseling and support around body image issues, individuals pursuing non-surgical methods often experience improvements in quality of life measures similar to those who undergo surgery.
How to fix diastasis recti without surgery?
There are a variety of approaches to healing diastasis recti without surgery, but all physical therapy and targeted exercise techniques will have in common a focus on better managing intra-abdominal pressure.
A comprehensive, holistic DR rehab protocol will include:
- A focus on establishing optimal breathing patterns, both relaxed and underload
- Exercises that help the patient learn to appropriately engage the core during movement, beginning with low load and progressively increasing
- Exercises integrating the transverse abdominal muscles with the other core musculature, including the rectus abdominis muscles
- Exercises that help patients increase the mobility and strength of the whole body, especially including shoulders, hips, and pelvic floor
- Coaching or counseling on relevant body image/mental health issues
It is surprisingly difficult to make an exhaustive list of exercises that have been shown through studies to effectively improve diastasis recti–there is no consensus in the literature. However, there is plenty of evidence that both practicing activation of the transverse abs and coordinating the use of the rectus abdominis with other muscle groups can have a positive effect on DR. Getting patients to train their core to be responsive to load requires giving plenty of opportunities for core engagement beyond supine exercises.
Your patients should look for providers or programs that offer a whole-body or holistic approach to diastasis recti healing. Exercise programs should be tailored to various stages of your patient’s recovery, with an emphasis on customization based on assessment. While most cases of diastasis recti have common aspects, each person’s body is unique and responds uniquely to exercise. Therefore, ongoing progress assessment is essential for effectively restoring core function.
Lifestyle Factors Affecting DR healing
Diastasis recti healing involves supporting both connective tissue and muscle development. Giving nutritional advice is outside my scope as a movement teacher; promoting overall good nutrition, adequate protein intake, and hydration is important. Use your expertise in guiding your patients.
Other environmental modifications that may enhance patient outcomes include incorporating walking daily and finding novel positions and options for sitting and standing (again, this might be better suited for a movement professional or PT). Your patients may need to adapt some of the ways they perform daily living activities to accommodate the healing process. Referring to a pelvic health occupational therapist or a specialized movement instructor may be beneficial in such cases.
What to Tell Your Patients Who Have Diastasis Recti
As an expert in your field, you are well-positioned to assist patients who are concerned about a weak core. Begin by thoroughly assessing their physical condition and based on your findings, referring them to the appropriate professional to help them design and implement a core rehabilitation program. Emphasize that diastasis recti responds incredibly well to non-surgical treatments. Additionally, assess the impact on their mental health and body image and refer them to relevant professionals as needed. Most importantly, it’s crucial to remind your patients that healing takes time and commitment and that they deserve to feel comfortable and confident in their body.

FAQ section:
1. What are the latest diagnostic criteria for identifying diastasis recti in patients?
The latest diagnostic criteria for diastasis recti involve measuring the inter-recti distance (IRD). This is typically done using calipers, ultrasound imaging, or manual palpation. A gap of more than 2.7 cm between the rectus abdominis muscles at the level of the umbilicus is generally considered diagnostic. Some guidelines also include a functional assessment of the abdominal wall to evaluate any associated weaknesses or dysfunctions.
2. How does the effectiveness of non-surgical interventions compare with surgical options in long-term studies?
Long-term studies suggest that non-surgical interventions, such as physical therapy and targeted exercises, can be effective in reducing the severity of diastasis recti and improving functional outcomes. However, surgical options tend to provide more significant anatomical corrections, especially in severe cases.
3. Which specific physical therapy techniques have shown the most promise in diastasis recti repair?
The most promising physical therapy techniques for diastasis recti include deep core stability exercises, pelvic floor exercises, guided breathing practices, and functional training that focuses on the transverse abdominis and oblique muscles.
4. How can professionals effectively tailor exercise programs to individual diastasis recti patient needs and recovery stages?
Professionals can tailor exercise programs by conducting thorough assessments to understand the severity of the diastasis, the patient’s overall physical condition, and any coexisting conditions. Programs should start with low-impact exercises focusing on core stability and gradually progress to more advanced movements as the patient gains strength and control. Regular reassessment and patient feedback are crucial for adjusting the intensity and type of exercises appropriately.
5. What are the most common challenges in non-surgical diastasis recti repair, and how can they be addressed?
Common challenges include patient compliance, variability in the severity of diastasis, and difficulty in maintaining correct form during exercises. These can be addressed by providing clear, personalized instructions, using visual aids or mirrors for feedback, and offering regular follow-ups to ensure adherence and proper technique. 1-1 support from physical therapists or movement instructors can also improve outcomes.
6. What are the key factors in deciding between surgical and non-surgical treatment pathways for a patient?
Key factors include the severity of the diastasis, patient symptoms (such as pain or loss of function), cosmetic concerns, and the patient’s overall health and lifestyle. Non-surgical treatments are generally preferred for mild to moderate cases.



