Learn

Hi! I'm Lauren.
Nice to meet you
Lauren Ohayon is the creator of Restore Your Core® (RYC®), a comprehensive and sustainable whole-body fitness program that empowers women to achieve ideal pelvic floor / core function and be strong, long, mobile and functional.

Hi! I'm Lauren.
Nice to meet you
Top articles
Is Pelvic Floor Repair Major Surgery? | Pelvic Health Guide

Pelvic floor repair surgery is the most common surgery for pelvic organ prolapse. Pelvic floor repair is a broad term used to classify a variety of simple, surgical procedures for repairing the pelvic floor. The three surgeries for pelvic floor prolapse include: anterior repair, posterior repair, and a hysterectomy.
Although Restore Your Core does not provide any surgical treatment for pelvic floor issues, my hope is that this article may answer any questions you may have regarding pelvic floor repair and the various procedures and treatments involved in getting you back to a healthy, active lifestyle.
Start your healing today with this free workout
Table of Contents
What are the Symptoms of Pelvic Organ Prolapse?
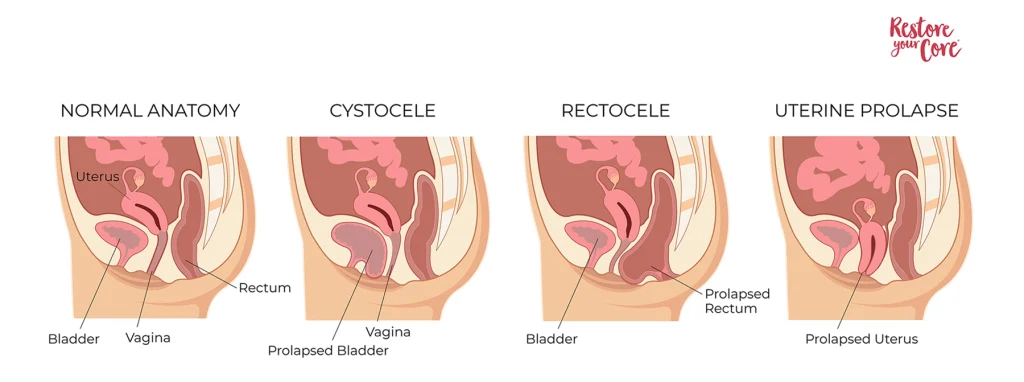
Prolapse can affect several abdominal organs. These organs are said to prolapse if they descend into or out of the vaginal canal or anus. The medical terminology for these occurrences include:
- Cystocele: prolapse of the bladder into the vagina, the most common condition
- Urethrocele: prolapse of the urethra (the tube that carries urine)
- Uterine prolapse
- Vaginal vault prolapse: prolapse of the vagina
- Enterocele: Small bowel prolapse
- Rectocele: Rectum prolapse
What Causes Pelvic Organ Prolapse?
There are many factors that are thought to cause a prolapse. In most cases, anything that may apply or put increased pressure in the abdomen can lead to a pelvic organ prolapse. Some of the common causes may include:
- Pregnancy, labor, and childbirth are the most common causes
- Obesity
- Connective tissue disorders
- Respiratory problems with a chronic, long-term cough
- Constipation
- Genetic factors
- Pelvic organ cancers
- Surgical removal of the uterus (hysterectomy)
- Diastasis recti (weakened core, connective tissues)
Symptoms
The symptoms of a prolapse somewhat depend on which organ has descended. If you are suffering from a bladder prolapse, urinary incontinence may occur. If it is a rectal prolapse, constipation, painful bowel movements, and painful sex often occur. Lower back pain, painful sex, and bowel obstruction or incontinence tend to accompany a small intestine prolapse as well. If you are suffering from a prolapse of the uterus, you may also suffer from uncomfortable intercourse, incontinence, and lower back pain.
In some cases, there may never be signs of a prolapse or the presence of any painful symptoms. However, in others some women report symptoms ranging from:
- Pressure or sense of fullness in the pelvic area
- Lower back pain
- Painful sex
- Sensation of something falling out of the vagina
- Urinary incontinence or frequent urination
- Constipation
- Spotting or bleeding from the vagina
In cases where there may be a severe prolapse, POP symptoms may worsen. One may notice:
- Bulging of the vaginal region
- Needing manual assistance during a bowel movement
- Difficulty urinating, spraying stream of urine
- The need to lift the bulging vagina in order to urinate
- Urinary leakage during intercourse
- Recurrent UTIs or kidney infections
How long does a pelvic floor repair operation take?
The length of the surgical procedure can vary greatly from patient to patient. The general estimate for the surgery ranges from around 3-5 hours, but may have a shorter or longer duration depending on various factors. Some of the elements that may determine the length of the operation can include:
- Internal anatomy
- Shape of the pelvis
- Weight
- Internal scarring or inflammation
- Prior abdominal/pelvic floor surgery
Does Surgery Really Work?
Surgery to fix a uterine prolapse are usually successful. In most patients the surgeries for POP have been reported to have an 80% – 95% success rate.
The success rate for sacrospinous ligament fixation (surgery to correct the bulging of the vagina) ranges between 80% – 90%, for uterosacral ligament suspension (surgery restoring support to the top of the vagina) is also 80%-90% successful, and sacrocolpopexy (surgery fixing the vaginal vault and the cervix) and sacrohysteropexy (fixing the prolapse of the uterus) have also shown the same success rate.
However, even after prolapse surgery, there is still a chance that another part of the vagina or uterus may prolapse.
Try 18 minutes of healing, nourishing movement – the RYC® way

What Can I Expect After POP Surgery?
These are the general guidelines that doctors will usually give post POP OP (this is not medical advice): Each day in recovery you can expect to begin to feel stronger. During your recovery, you may need to remain on pain medication for about a week or two and may experience fatigue and weakness. A typical recovery time line varies from 4 to 6 weeks until you recover from an open surgery and anywhere from 1 to 2 weeks to recover from vaginal surgery. Your doctor should give you more specific guidelines.
During your recovery period, you should avoid any sexual activity, vigorous exercise, heavy lifting, or any activities that may put pressure or strain your operation area. Your doctor should give you more specific guidelines. The most important aspect to your quick recovery is rest – getting enough sleep will help you recover.
During your recovery, you might experience vaginal discharge or light bleeding. If so, avoid using tampons or douche. Use a sanitary pad if necessary. Your doctor should give you more specific guidelines.
How long do you stay in the hospital after prolapse surgery?
After your prolapse surgery, it is likely that you will need to remain hospitalized for 2 – 3 days depending on the operation and any underlying medical conditions you have. During this time your medical care takers will help ensure your recovery by monitoring for any potential complications and providing clean, sanitized treatment of the operation site.
Are There Complications with Prolapse Surgery?
Although pelvic surgery has proven to be a very safe procedure, as with any surgery, there are a few risks and potential complications that can arise. Please discuss this with your doctor but the common ones include:
- Bleeding
- Infection
- Tissue or organ injury
- Hernia
- Conversion to open surgery
- Urinary incontinence
- Urinary retention
- Vesicovaginal fistula (rare, abnormal connection between vagina and bladder)
If you are experiencing any of these symptoms of complications, it is important that you seek medical assistance. In some cases these symptoms can be common and unserious, but it is always best to consult your doctor if you have any concerns.
Enjoy a free, pelvic-floor & core healing whole-body workout today
Can pelvic floor muscles be repaired?
If you have experienced a prolapse, uterine or otherwise, it can be a shocking and painful experience. However, there are ways to decrease symptoms without surgery.
Nonsurgical Treatments
There are several ways in which to treat a uterine or vaginal prolapse. The three most common approaches are pessary, restorative exercises, and biofeedback therapy.
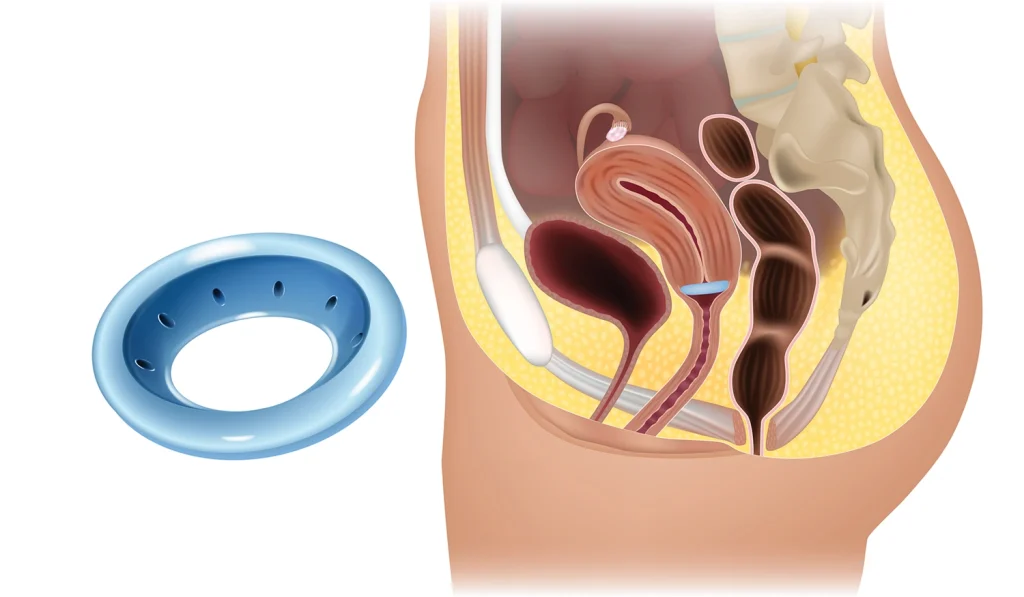
Pessary
A pessary is probably one of the first treatments your doctor will recommend if you have symptoms of POP. A pessary is a ring shaped device that is inserted into your vagina. This will help support your pelvic organs. Being fitted for a pessary is a lot like being fitted for a diaphragm. Many of my clients with severe POP find that a pessary is useful for allowing them to live fuller lives while they slowly use PT and exercise to help resolve the prolapse.
Restorative Exercises & Physical Therapy
Pelvic floor exercises help strengthen your pelvic muscles. Although the most common exercise recommended by health professionals today is the kegel exercise, there are many more exercises that you can do that are helpful for restoring PF function and giving support for your pelvic organs. Kegels are a pretty outdated model of care when used alone, without a more whole body approach to healing.
What is involved in pelvic floor reconstruction?
Pelvic floor reconstruction surgery is a group of procedures that are performed to treat prolapse of uterus, rectum, small intestines, or other pelvic organs.
Anterior Vaginal Repair
Anterior repair is a surgical procedure that seeks to reinforce weakened layers between the bladder and the vagina. This surgery helps relieve symptoms such as vaginal bulging and to improve bladder function.
The surgery can be performed under general anaesthetic. The most common method of anterior repair is by an incision made along the centre of the front wall of the vagina – starting at the entrance and ending at the top of the vagina. The weakened layers are then repaired and anu superfluous tissue is removed. This is typically done with absorbable stitches.
Posterior Vaginal Repair
A back wall (posterior) vaginal prolapse is usually caused by weakness in the tissues and muscles that divide the vagina from the lower part of the bowel. This surgical procedure is performed to order to repair or restore the weakened layers between the rectum and the vagina.
As with an anterior vaginal repair surgery, posterior repair surgery is usually performed under general anesthetic. The procedure involves a minor incision being made along the back wall of the vagina starting at the entrance and finishing near the top. The weakened layers are then repaired using absorbable stitches.
Vaginal Hysterectomy
A vaginal hysterectomy is typically performed with a prolapsed uterus. This is when the uterus (womb) descends into the vagina and in some severe cases, protrudes or extends outside of the vaginal canal. The surgery is performed by removing the uterus through the vagina.
A vaginal hysterectomy is performed under general or spinal anaesthetic. In order to remove the uterus, the surgeon will make an incision at the top of the vagina around the cervix, clears the bowel and bladder from the uterus, and cuts through the connecting tissues to remove the uterus. The surgeon will then close the vaginal vault and commonly adds additional supporting stitches as the surgery is being performed.
Does Physical Therapy Help Post-Surgery?
If you are meeting with a physical / occupational therapist or taking part in a rehabilitation program such as Restore Your Core® post-surgery, some of the common exercises and techniques consist of:
Posture:
Spine, pelvis, and hip alignment is necessary for a sustained recovery. Being mindful of good posture will help relieve any additional strain or pressure you apply to your pelvic region.
Restful Poses:
These poses are positions which utilize gravity to encourage the pelvic organs to be “repositioned” back into the pelvic cavity.
Lower abdominal Exercises:
This involves contracting the lower abdominal muscles while practicing dynamic and static exercises. If done correctly, it can limit the stress placed on the interior organs during activities which increase intra-abdominal pressure (i.e. squats).
PFM Strengthening:
PFM strengthening exercises are a great way to help get your body back to its normal function and to heal from POP surgery. I advise getting instruction from a pelvic floor specialist who is trained in assessing the whole person to determine the appropriate exercise routines for you.

In my program, Restore Your Core®, I cover many helpful exercises and routines that can help heal POP and any abdominal or core issues. To learn more about restorative exercises for uterine prolapse or other abdominal issues, consider checking out one of my previous blog posts on core workouts and exercises.
Access your free workout and start healing your core and pelvic floor today
Top articles
“There is no thank you big enough for Lauren Ohayon existing and thinking and helping so many of us. Every time I do something I never thought I’d do again she is part of the reason why.”
Laura Gregg
Strengthen, heal & nourish your pelvic floor & core
Try a FREE workout
with Lauren
*10K+ women healed and healing

Thank you!
Your FREE video is on the way
Please check your email inbox in a few minutes.

Related articles



Your pelvic floor muscles play an important part for many bodily functions, including sexual health and orgasms. In this article, I’m debunking common myths about your pelvic floor and highlighting...





Enjoy a free, pelvic-floor & core healing whole-body workout today
Get more actionable info, inspiration and exclusive offers delivered to your inbox.
*No spam, just quality content and support
Thanks for subscribing!
inbox soon.
Thanks for subscribing!
Please check your inbox soon.

Strengthen, heal & nourish your pelvic floor & core
Try a FREE workout
with Lauren
*10K+ women healed and healing

Thank you!
Your FREE video is on the way
Please check your email inbox in a few minutes.




